German coronavirus patient feels 'lucky' to be treated with world-class care
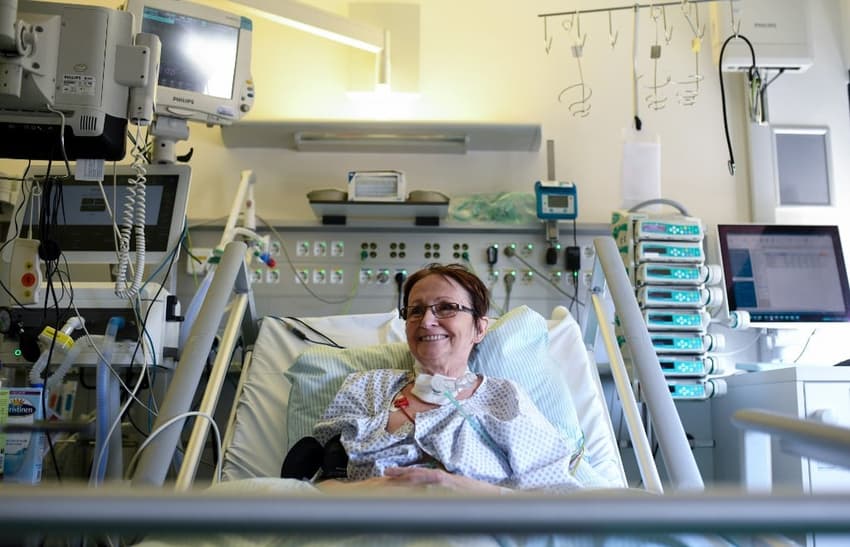
Despite a high number of infections, the death toll from the coronavirus in Germany has been much lower than in France, Italy or the United States. Experts have credited Berlin for widespread testing and ample capacity for infected patients.
After making it through the first night breathing on her own, 60-year-old Martina Hamacher can only say: "I've been lucky."
One of Germany's earliest coronavirus patients, Hamacher is still tangled in some of the tubes and cables that helped keep her alive for 20 days in intensive care.
"I've made it this far," she says with a slight smile in Aachen's university hospital.
Things could have been worse for Hamacher had she not been treated in Germany, where the response to the crisis has been internationally admired.
Despite a high number of infections, the death toll has been much lower than in France, Italy or the United States. Experts have credited Berlin for widespread testing and ample capacity for patients stricken with the respiratory illness.
Such large-scale efforts appear to have paid off, with patients receiving world-class care by medical staff who have stayed on top of the crisis.The hospital in Aachen has even been able to take patients from Belgium and the Netherlands.
"I'm very grateful for what the doctors and nurses did, without them I don't think I'd still be here," Hamacher says.
'Doing our duty'
Sleeping patients unable to survive without assistance can be seen through yellow sliding doors that open into two-bed intensive care units (ICU) at the hospital.
Amid constant beeping at different pitches and volumes from life-support machines, doctors and nurses work in their epidemic armour of masks, gloves, caps and protective suits.
"This is part of our duty that we're living up to," said a nurse named Kathi.
Aachen has 51 coronavirus patients at present, 35 of them in intensive care.
"It's important to me that this isn't only tied up with death and technology," says ICU director Gernot Marx.
"We bring most people back to life, not because of all the machines we have but because of people who know what they're doing, who commit themselves so strongly."
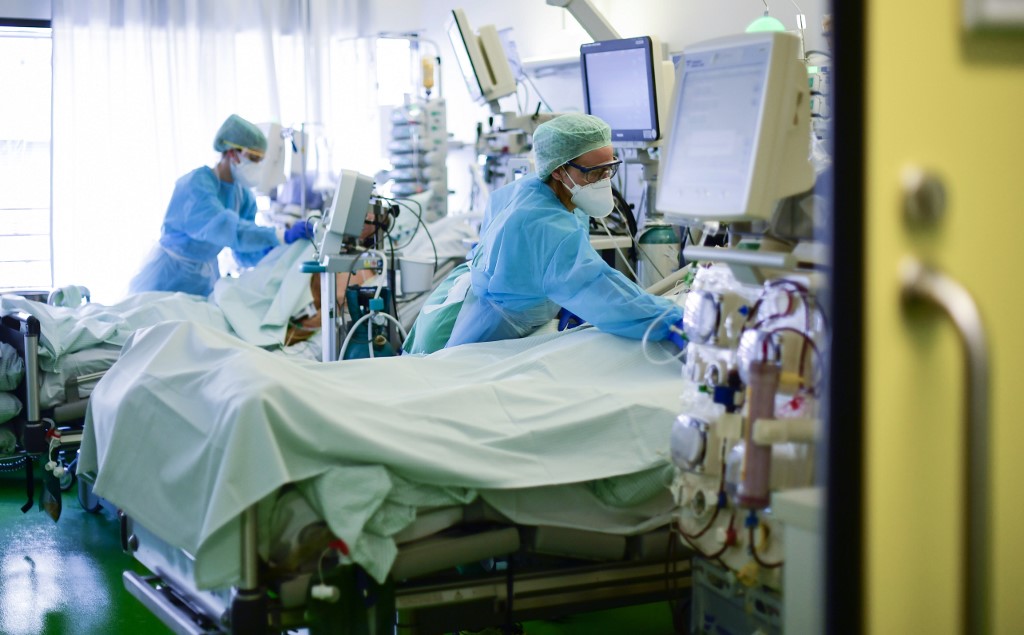
Medical staff take care of Covid-19 patients in an intensive care unit at the University hospital of Aachen, wester Germany on April 15, 2020: AFP
The Aachen hospital's experience with coronavirus began slowly, Marx recounts.
"We understood that we could and must use the time to prepare, because the images from Bergamo (in northern Italy) were horrifying. We were determined not to let that become the reality here."
Within a few days, the number of ICU beds surged from 96 to 136, an increase matched by other German medical facilities.
A further 70 places could be quickly set up if needed, but the country already had 11,000 free intensive care beds from a nationwide total of 25,000. "We were always prepared to take people in," Marx says.
More than 3,800 people have died in Germany out of more than 133,000 confirmed infections, a rate well below other big European Union countries such as France or Spain.
And since April 12, more people have been declared disease-free each day than new infections have been reported, Health Minister Jens Spahn said Friday.
'Life is good'
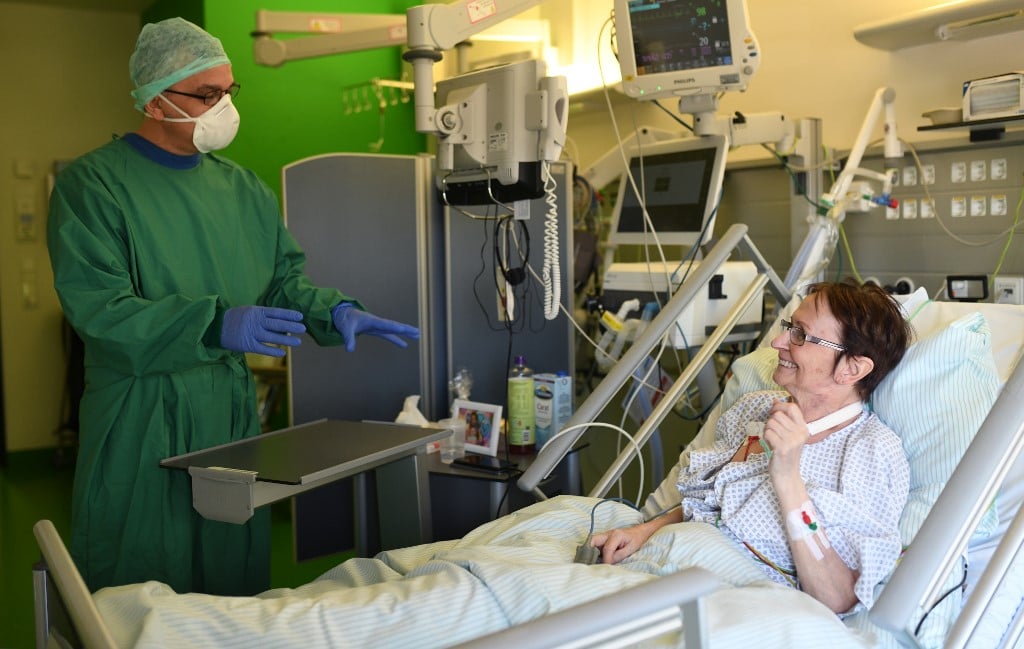
Covid-19 patient Martina Hamacher talks to a nurse at the weaning ward of the University hospital of Aachen, wester Germany on Apeil 15, 2020.
Hamacher recalls that "all of a sudden, the virus was in our corner of the world". One day, "I felt a little weak, as if I was getting the flu, and I had a slight fever."
When the sickness intensified, "I've never experienced anything like it," she adds. "This sensation of not being able to breathe, it's impossible to describe, it will always be in my head."
But leaving the ICU is only the first step on a long path back to full health.
Time spent on a ventilator "damages our lungs, even if we've saved a life, we don't have normal breathing afterwards," says Anne Bruecken, head of a "weaning" unit for patients coming off the machines.
After potentially weeks of breathing assistance, people "don't get off ventilation easily," Bruecken explains, but need one or two more weeks toachieve independent respiration.
"We have muscles that we normally use to breathe, and the longer we ventilate, the weaker they become."
Some patients must even "learn how to swallow again," Bruecken notes. They then often spend more time in rehab centres.
Meanwhile, Hamacher's new room is brightened up with drawings by her grandchildren.
Staff must still wear protective gear, and visits are strictly forbidden.
"It would be nicer if someone would come now and then, it's been a long time already, especially for the grandkids," Hamacher says.
Despite everything, "I feel like a queen today, I can tell that things are getting better," she says with a smile.
"Life is good, whatever comes next, I'll have to enjoy it!"
Comments
See Also
After making it through the first night breathing on her own, 60-year-old Martina Hamacher can only say: "I've been lucky."
One of Germany's earliest coronavirus patients, Hamacher is still tangled in some of the tubes and cables that helped keep her alive for 20 days in intensive care.
"I've made it this far," she says with a slight smile in Aachen's university hospital.
Things could have been worse for Hamacher had she not been treated in Germany, where the response to the crisis has been internationally admired.
Despite a high number of infections, the death toll has been much lower than in France, Italy or the United States. Experts have credited Berlin for widespread testing and ample capacity for patients stricken with the respiratory illness.
Such large-scale efforts appear to have paid off, with patients receiving world-class care by medical staff who have stayed on top of the crisis.The hospital in Aachen has even been able to take patients from Belgium and the Netherlands.
"I'm very grateful for what the doctors and nurses did, without them I don't think I'd still be here," Hamacher says.
'Doing our duty'
Sleeping patients unable to survive without assistance can be seen through yellow sliding doors that open into two-bed intensive care units (ICU) at the hospital.
Amid constant beeping at different pitches and volumes from life-support machines, doctors and nurses work in their epidemic armour of masks, gloves, caps and protective suits.
"This is part of our duty that we're living up to," said a nurse named Kathi.
Aachen has 51 coronavirus patients at present, 35 of them in intensive care.
"It's important to me that this isn't only tied up with death and technology," says ICU director Gernot Marx.
"We bring most people back to life, not because of all the machines we have but because of people who know what they're doing, who commit themselves so strongly."

Medical staff take care of Covid-19 patients in an intensive care unit at the University hospital of Aachen, wester Germany on April 15, 2020: AFP
The Aachen hospital's experience with coronavirus began slowly, Marx recounts.
"We understood that we could and must use the time to prepare, because the images from Bergamo (in northern Italy) were horrifying. We were determined not to let that become the reality here."
Within a few days, the number of ICU beds surged from 96 to 136, an increase matched by other German medical facilities.
A further 70 places could be quickly set up if needed, but the country already had 11,000 free intensive care beds from a nationwide total of 25,000. "We were always prepared to take people in," Marx says.
More than 3,800 people have died in Germany out of more than 133,000 confirmed infections, a rate well below other big European Union countries such as France or Spain.
And since April 12, more people have been declared disease-free each day than new infections have been reported, Health Minister Jens Spahn said Friday.
'Life is good'

Covid-19 patient Martina Hamacher talks to a nurse at the weaning ward of the University hospital of Aachen, wester Germany on Apeil 15, 2020.
Hamacher recalls that "all of a sudden, the virus was in our corner of the world". One day, "I felt a little weak, as if I was getting the flu, and I had a slight fever."
When the sickness intensified, "I've never experienced anything like it," she adds. "This sensation of not being able to breathe, it's impossible to describe, it will always be in my head."
But leaving the ICU is only the first step on a long path back to full health.
Time spent on a ventilator "damages our lungs, even if we've saved a life, we don't have normal breathing afterwards," says Anne Bruecken, head of a "weaning" unit for patients coming off the machines.
After potentially weeks of breathing assistance, people "don't get off ventilation easily," Bruecken explains, but need one or two more weeks toachieve independent respiration.
"We have muscles that we normally use to breathe, and the longer we ventilate, the weaker they become."
Some patients must even "learn how to swallow again," Bruecken notes. They then often spend more time in rehab centres.
Meanwhile, Hamacher's new room is brightened up with drawings by her grandchildren.
Staff must still wear protective gear, and visits are strictly forbidden.
"It would be nicer if someone would come now and then, it's been a long time already, especially for the grandkids," Hamacher says.
Despite everything, "I feel like a queen today, I can tell that things are getting better," she says with a smile.
"Life is good, whatever comes next, I'll have to enjoy it!"
Join the conversation in our comments section below. Share your own views and experience and if you have a question or suggestion for our journalists then email us at [email protected].
Please keep comments civil, constructive and on topic – and make sure to read our terms of use before getting involved.
Please log in here to leave a comment.